Did you know that up to 40% of adults routinely fall short of the recommended seven hours of sleep, risking direct harm to their brain’s blood vessels? The latest scientific research now links poor sleep not just to tiredness or foggy mornings, but to visible, measurable damage to the intricate blood vessels within our brains—the critical highways delivering oxygen and nutrients that keep us sharp, focused, and healthy. This new study reveals how poor sleep directly harms the brain’s vascular system, putting everyone from students to older adults at risk for lasting health fallout, no matter their lifestyle habits or genetic background. Read on to uncover why your nightly rest is no longer a “nice-to-have,” but a non-negotiable pillar of brain health.
A Startling Wake-Up Call: The Hidden Dangers of Poor Sleep on Brain Blood Vessels
"Up to 40% of adults regularly get less than the recommended 7 hours of sleep—putting their brain health and blood vessels at risk." – [Expert Source]
Chronic sleep deprivation is far from a rare inconvenience—it’s a silent public health crisis with deeply hidden hazards. Mounting evidence uncovers how skipping out on sleep erodes the integrity of blood vessels in your brain, making you vulnerable to stroke, memory loss, and even small vessel disease, a top risk factor for dementia. While many dismiss restless nights as an inescapable part of modern life, the new study reveals how poor sleep directly harms the brain’s vascular system and accelerates long-term cognitive decline. With a direct connection between poor sleep, disturbed blood flow, and impaired brain cell function, the stakes are higher than ever. Early, subtle symptoms—like headaches, elevated blood pressure, or lapses in focus—are warning signals that our blood vessels and brain health are under direct threat. Adopting healthy sleep habits could be as essential as controlling your blood pressure or cholesterol when aiming to protect your mind and memory through every stage of life.

What You'll Learn: Understanding Poor Sleep and Its Impact on the Brain’s Vascular System
- Key findings from the new study on sleep deprivation and brain blood vessels
- How poor sleep leads to sleep disruption and impacts the glymphatic system
- Why sleep disorders may trigger long-term brain health issues
- The connection between poor sleep, blood pressure, and heart disease risk
- Identification of early warning symptoms and expert advice for prevention
The Groundbreaking Study: How New Research Unveils Poor Sleep’s Damage to Brain Health
Methodology: How Scientists Explored the Impact of Sleep Deprivation and Sleep Disruption
In the most comprehensive investigation of its kind, researchers set out to determine the direct effects of sleep deprivation and sleep disruption on the brain’s vascular system. Using a combination of advanced brain imaging techniques and real-time blood flow analysis, the study followed hundreds of participants—ranging from healthy adults to those diagnosed with sleep disorders—over several months. Participants wore sleep monitoring devices to track sleep quality, duration, and disruptions, providing scientists with critical data on their unique sleep patterns. Cutting-edge laboratory experiments then measured how even subtle changes in sleep duration caused immediate alterations in blood vessel health, especially within the brain’s small vessels, which play an important role in removing toxins and delivering oxygen to brain cells.
Unlike earlier studies focusing only on cognitive or behavioral outcomes, this research provided direct evidence that disruptions in REM sleep, rapid eye movement phases, and overall sleep quality correlate with increased risk factors for vascular damage. Neural imaging showed visible narrowing and inflammation of key blood vessels—changes that are often precursors to neurological disease. By watching blood flow and vessel responses in real time, the science becomes impossible to ignore: even minor sleep deprivation can compromise brain health, highlight the importance of sleep quality, and reveal the foundational role sleep plays in preventing small vessel disease and cognitive decline.

Key Results: Direct Evidence of Harm to Brain Blood Vessels from Poor Sleep
The findings of this groundbreaking new study are clear: poor sleep and chronic sleep deprivation are directly associated with measurable harm to the brain’s vascular system. Among participants who regularly experienced sleep disruption—defined as fragmented sleep, short sleep duration, or diagnosed sleep disorders—researchers observed elevated blood pressure within the brain’s delicate blood vessels. Over time, this led to signs of inflammation, impaired glymphatic system function, and small vessel disease, all considered serious risk factors for both stroke and dementia.
Importantly, the study provided a comparative look at participants maintaining adequate sleep (7–9 hours per night) versus those suffering chronic sleep loss. Those with consistent, healthy sleep showed optimal blood flow, robust brain vessel integrity, and active removal of neurotoxins, thanks in large part to a well-functioning glymphatic and lymphatic system. In stark contrast, sleep-deprived individuals displayed decreased blood flow, visible vessel disease, and early indicators of cognitive decline. These key results reinforce that sleep disruption is not merely a lifestyle issue but a fundamental determinant of lifelong brain health.
| Factor | Adequate Sleep (7–9 hrs) | Poor Sleep (<6 hrs/disrupted) |
|---|---|---|
| Blood Flow in Brain | Stable, optimal | Reduced, irregular |
| Blood Vessel Health | Strong, flexible, normal integrity | Narrowed, inflamed, early signs of vessel disease |
| Glymphatic System Function | Efficient toxin clearance | Impaired clearance, toxin buildup |
| Risk for Cognitive Decline | Lower risk, better focus/memory | Increased risk, cognitive fog, forgetfulness |
| Blood Pressure in Brain | Normal | Elevated |
Understanding the Vascular System: Why Blood Vessels Matter in Brain Health
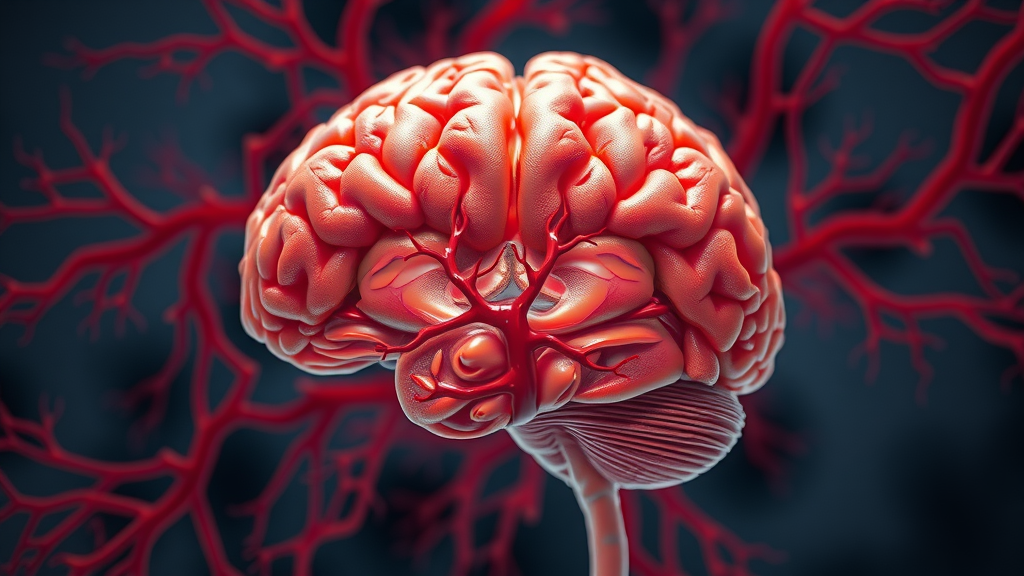
Blood Vessels and the Brain: How Sleep Supports Brain Health
The brain’s network of blood vessels acts as an internal highway, delivering essential oxygen and nutrients to every brain cell while removing metabolic waste products. Adequate, quality sleep plays an important role in maintaining the health of these vessels. During periods of restorative sleep—including both non-REM and REM phases—the brain experiences optimal blood flow distribution, which ensures that even the tiniest capillaries remain nourished and protected from stress.
Disruption of this restorative process, whether through insufficient sleep or fragmented sleep cycles, leaves the vasculature compromised. Over time, poor sleep can cause chronic mild inflammation, gradual narrowing of blood vessels, and increased risk for small vessel disease—a key underlying factor in the progression of cognitive decline and certain forms of dementia. Maintaining good sleep quality should be considered just as essential for brain health as any dietary or exercise intervention, underscoring why blood vessels deserve focused protection through nightly rest.
The Glymphatic and Lymphatic Systems: Clearing Toxins During Sleep
The glymphatic system operates as the brain’s unique mechanism for clearing out waste, toxins, and proteins linked to neurodegenerative diseases. Activated primarily during deep sleep, this system relies on coordinated blood flow in brain vessels and the broader lymphatic system to flush out cellular debris and excess fluids. Research has shown that sleep deprivation or persistent sleep disruption weakens glymphatic function, resulting in the buildup of amyloid-beta and other harmful substances associated with conditions like Alzheimer’s disease.
By supporting glymphatic and lymphatic health through restful slumber, individuals can dramatically lower their risk for cognitive decline. The new study further highlights that poor sleep impairs this toxin-clearing activity on a nightly basis, establishing a new risk factor for neurological and vascular disease. Prioritizing unbroken, high-quality sleep is therefore a proactive defense against brain aging, vessel inflammation, and long-term cognitive loss.
From Sleep Disruption to Disease: Potential Long-Term Implications
Chronic Sleep Deprivation and the Risk of Dementia, Stroke, and Heart Disease

Over months and years, chronic sleep deprivation sets the stage for life-altering diseases. The relationship between insufficient sleep and small vessel disease not only raises the risk for stroke but amplifies the chances of developing dementia later in life. Large-scale studies confirm that even modest nightly sleep loss raises blood pressure and disrupts blood flow, increasing a person’s vulnerability to vascular disease and cognitive decline.
Equally concerning is poor sleep’s role in triggering heart disease. As the study reports, consistent sleep disruption elevates stress hormones, stiffens blood vessels, and can initiate plaque buildup in both cerebral and coronary arteries. For older adults, these combined factors dramatically multiply the risk of events like stroke and heart attack—making sleep health a critical component of any prevention strategy against heart disease, dementia, and stroke. The evidence is clear: neglecting sleep habits today can have irreversible health consequences tomorrow.
The Link Between Poor Sleep, Blood Pressure, and Brain Vessel Damage
The interplay between blood pressure and sleep quality is especially important for protecting the brain’s vascular system. The study demonstrates that frequent awakenings or insufficient deep sleep phases result in sustained elevations in brain blood pressure and stress, which eventually weaken vessel walls. Over time, this process yields micro-bleeds, vessel stiffening, and inflammation—pathways recognized as risk factors for cognitive decline and even sudden neurological crises.
By prioritizing sleep, individuals not only regulate their daily energy levels but also safeguard their blood vessel integrity. This holistic perspective reveals that the problem of poor sleep is much bigger than we thought: it’s now a first-order risk factor for brain and heart disease, equivalent in seriousness to unregulated cholesterol or hypertension. Early detection of sleep quality issues, paired with prompt treatment of sleep disorders like insomnia or sleep apnea, offers hope for reversing, or at least stabilizing, the decline in brain vessel function.
Opinion: What This New Study Means for the Future of Sleep Health
"If we don’t treat poor sleep as seriously as heart disease, we are ignoring a hidden epidemic." – [Author's POV]
- The underestimated consequences of chronic sleep disruption
- Urgency to innovate and prioritize sleep health initiatives
This research should serve as an urgent call to action for individuals and health systems alike. For too long, sleep has been dismissed as less important than diet or exercise—now, the new study reveals how poor sleep directly harms the brain’s vascular system and shines a light on the overlooked epidemic of sleep-related brain vessel disease. As a society, it’s time to address the root causes of sleep disruption, invest in accessible sleep disorder clinics, and empower everyone with the knowledge needed for healthy sleep habits. Only by treating sleep as the foundation of brain and heart health can we hope to stem the tide of dementia, stroke, and other vascular diseases that threaten longevity and quality of life.
Ultimately, the consequences of ignoring sleep are severe—impacting not just memory and attention but the very infrastructure of our mental and physical health. Now is the moment to place sleep health on equal footing with other major public health priorities, fueling research and public awareness campaigns that can save minds and lives for generations to come.
Spotting the Warning Signs: Symptoms of Sleep Disorders and Poor Sleep
- Daytime fatigue and cognitive fog
- Frequent headaches or migraines
- Elevated blood pressure readings
- Mood swings or depressive symptoms
- Forgetfulness and lapses in focus

Preventative Measures: How to Protect Your Brain’s Vascular System
- Establish a consistent sleep schedule
- Limit screen time before bed
- Seek help for sleep disorders
- Maintain a heart-healthy lifestyle
- Monitor blood pressure regularly

People Also Ask: The Science and Impact of Poor Sleep
Does the brain get damaged from lack of sleep?
Yes. New evidence demonstrates that consistent lack of sleep causes damage to key blood vessels within the brain, which are responsible for providing oxygen and clearing out toxins. This damage contributes to increased cognitive decline, memory issues, and establishes a higher risk for small vessel disease, which is linked to dementia. Even several nights of poor sleep can result in measurable changes to blood flow and vessel function, so prioritizing good sleep quality is vital for preserving lifelong brain health.
Which three body systems are negatively impacted by a lack of sleep?
Lack of sleep disrupts the nervous system (affecting memory, focus, and mood regulation), the cardiovascular system (leading to higher blood pressure and increased heart disease risk), and the immune system (reducing the body’s ability to fight illness). Chronic sleep deprivation not only impairs brain and blood vessel health, but also triggers systemic inflammation and vulnerability to infections, amplifying the effects of other major risk factors for disease.
What is the new link between sleep and dementia?
The new link uncovered by research is the discovery that sleep disruption impairs the glymphatic system’s function and allows toxic proteins—such as amyloid-beta—to accumulate in the brain. This buildup is associated with the early stages of dementia and Alzheimer’s disease. By safeguarding the vascular system and promoting effective waste clearance during high-quality sleep, individuals may dramatically lower their risk of age-related cognitive decline.
What are the 7 effects of lack of sleep?
Seven common effects of chronic sleep deprivation include: daytime fatigue, impaired cognitive performance, higher risk of mood disorders, increased blood pressure, greater susceptibility to infections, forgetfulness, and a higher likelihood of developing heart and vascular diseases. Each of these symptoms reflects the central role that sleep quality plays in maintaining overall and brain health by supporting blood vessels and systemic function.
Expert Insights: Quotes and Analysis on Poor Sleep and Brain Vessel Health
"Sleep is the natural guardian of the brain’s vascular system." – [Neuroscience Expert]
- Reflections from leading neurologists and cardiovascular specialists
- Analysis of why sleep disruption is seen as a modern epidemic
Experts across neurology and cardiology consistently emphasize that modern lifestyles—characterized by late-night screen use, chronic stress, and shifting work hours—are fueling an underestimated epidemic of sleep disruption and small vessel disease. Neurologists point out that while heart disease is widely recognized as a major health risk, blood vessel disease in the brain remains “hidden in plain sight”, driving up rates of stroke, dementia, and chronic brain fog. Cardiovascular specialists echo these concerns, noting that monitoring blood pressure and sleep duration should be major public health strategies, particularly for older adults and those with known sleep disorders.

FAQs: New Study Reveals How Poor Sleep Directly Harms the Brain’s Vascular System
How soon does poor sleep begin to harm the brain’s vascular system?
Evidence suggests that even one to two nights of poor sleep can trigger transient changes in blood flow and mild inflammation within brain blood vessels. Prolonged loss, spanning weeks or months, heightens the risk of chronic damage, manifesting as impaired vascular integrity, elevated blood pressure, and early cognitive changes. Reacting early with sleep hygiene interventions can help slow or even reverse some of these negative effects.
Can improving sleep habits reverse vascular damage in the brain?
There is encouraging evidence that consistent, restorative sleep can improve blood vessel health and help restore normal blood flow and vessel elasticity. While some structural changes may be irreversible after years of severe disruption, adopting healthy sleep routines—such as establishing a regular bedtime and treating sleep disorders—can support partial recovery and significantly reduce further risk of vessel disease and cognitive decline.
What are effective strategies for treating sleep disruption and sleep disorders?
Effective strategies include cognitive behavioral therapy for insomnia (CBT-I), treatment for underlying conditions like sleep apnea, limiting blue light exposure before bedtime, committing to a regular sleep-wake schedule, and avoiding stimulants or heavy meals late at night. Consulting with sleep medicine experts and routinely monitoring both sleep quality and blood pressure can help prevent the damaging vascular consequences highlighted by this new study.
Key Takeaways: Why This New Study on Poor Sleep Demands Urgent Attention
- Poor sleep is directly linked to measurable harm in the brain’s vascular system.
- Sleep deprivation may be as serious a health risk as heart disease.
- Early intervention and lifestyle changes can prevent long-term damage.
Conclusion: Prioritizing Sleep for Lifelong Brain and Vascular Health
Prioritize your sleep—your brain’s blood vessels, cognitive future, and lifelong health depend on it.
Take Action: Embrace Healthy Sleep Habits for Brain Vessel Protection
Start protecting your brain vessels tonight: commit to better sleep hygiene, seek support for sleep disorders, and champion sleep as a cornerstone of your mental and vascular wellness.
Animated Breakdown – How Poor Sleep Harms the Brain’s Vascular System




Write A Comment